USMLE Reviewer (By Subscription)
Structure and Function
Simple cuboidal epithelium
The surface epithelium of the ovary is called the germinal epithelium.
-
In some areas, it may appear low columnar or flattened (squamous-like)
Important Clarification
Despite its name, the “germinal epithelium” does NOT give rise to germ cells (oocytes). The term is historical and somewhat misleading.
Embryologic Origin
-
Derived from the coelomic epithelium (mesothelium)
Clinical Relevance
This surface epithelium is important because:
-
Most epithelial ovarian cancers arise from this layer (or from inclusion cysts derived from it).
-
Repeated ovulation causes disruption and repair of this epithelium, which is thought to contribute to malignant transformation risk.
If you’d like, I can also review how this differs from the epithelium of the fallopian tube (a common board comparison).
-
Historically called “germinal epithelium” (misnomer — does not give rise to germ cells)
-
Continuous with the peritoneum
-
Beneath it is a dense connective tissue layer called the tunica albuginea
Histologic Type
-
It is composed of simple cuboidal epithelium
-
In some areas, it may appear low columnar or flattened (squamous-like)
Important Clarification
Despite its name, the “germinal epithelium” does NOT give rise to germ cells (oocytes). The term is historical and somewhat misleading.
Embryologic Origin
-
Derived from the coelomic epithelium (mesothelium)
Clinical Relevance
This surface epithelium is important because:
-
Most epithelial ovarian cancers arise from this layer (or from inclusion cysts derived from it).
-
Repeated ovulation causes disruption and repair of this epithelium, which is thought to contribute to malignant transformation risk.
[If you’d like, I can also review how this differs from the epithelium of the fallopian tube (a common board comparison).]
-
Content 2
Content 3
🧫 Histology of the Ovary
The ovary has three main components:
-
Surface (germinal) epithelium
-
Cortex
-
Medulla
1️⃣ Surface Epithelium
2️⃣ Cortex (Outer Region)
This is the functional portion of the ovary.
Contains:
-
Ovarian follicles at various stages
-
Dense stromal connective tissue
-
Corpora lutea and corpora albicantia
🔹 Follicular Development Stages
Primordial follicle
-
Primary oocyte (arrested in prophase I)
-
Surrounded by single layer of flattened follicular cells
Primary follicle
-
Cuboidal granulosa cells
-
Formation of zona pellucida
Secondary (antral) follicle
-
Fluid-filled antrum
-
Theca interna (steroid-producing, LH-responsive)
-
Theca externa (fibromuscular support)
-
Granulosa cells (FSH-responsive)
Graafian (mature) follicle
-
Large antrum
-
Oocyte surrounded by corona radiata
-
Cumulus oophorus connects oocyte to granulosa layer
3️⃣ Corpus Luteum
-
Forms after ovulation
-
Large eosinophilic lutein cells
-
Secretes progesterone (and some estrogen)
-
If no pregnancy → degenerates into corpus albicans (fibrous scar)
4️⃣ Medulla (Inner Region)
-
Loose connective tissue
-
Blood vessels
-
Lymphatics
-
Nerves
-
No follicles normally present
🧠 High-Yield Summary
-
Cortex = follicles
-
Medulla = vessels
-
Theca interna → androgens
-
Granulosa → converts androgens to estrogen (via aromatase)
If you'd like, I can also give you a labeled exam-style diagram summary or correlate this with ovarian physiology across the menstrual cycle.
++++++++++++++++++++++++++++++++++++
-
- Covered by a layer called the germinal epithelium, a thin layer of simple cuboidal cells.
- Below the germinal epithelium lies the tunica albuginea, a dense connective tissue layer.
The ovary is divided into two regions:
-
Cortex:
- The outer region.
- Contains ovarian follicles in various stages of development:
- Primordial follicles.
- Primary follicles.
- Secondary follicles.
- Mature (Graafian) follicles.
- After ovulation, the remnants of a follicle form the corpus luteum, which secretes hormones.
- Over time, the corpus luteum degenerates into the corpus albicans.
-
Medulla:
- The inner region.
- Contains loose connective tissue, blood vessels, lymphatic vessels, and nerves.
- Provides structural support and nourishment to the cortex.
Blood Supply and Nerve Innervation
- Blood Supply:
- Provided by the ovarian arteries, which branch off the abdominal aorta.
- Venous drainage occurs via the ovarian veins.
- Nerve Supply:
- Sympathetic and parasympathetic fibers contribute to innervation, primarily for regulating blood flow and hormone secretion.

+++++++++++++++
Next is a cortex where the ovarian follicles can be found.
Ovarian follicles are oocytes surrounded by epithelial cells.
Included in the follicles are the cumulus oophorus, membrana granulosa, and the granulosa cells inside it, corona radiata, zona pellucida, and primary oocyte.
The zona pellucida, theca of follicle, antrum and liquor folliculi are also contained in the follicle. Also in the cortex is the corpus luteum derived from the follicles.
{A diagram of a sectioned ovary (a) shows the different stages of follicle maturation, ovulation, and corpus luteum formation and degeneration. All of the stages and structures shown in this diagram actually would appear at different times during the ovarian cycle and do not occur simultaneously. Follicles are arranged here for easy comparisons. The primordial follicles shown are greatly enlarged. The histologic sections identify primordial follicles (b), a primary follicle (c), a secondary follicle (d), and a large vesicular follicle (e). After ovulation, the portion of the follicle left behind forms the corpus luteum (f), which then degenerates into the corpus albicans (g). All H&E.]
+++++++++++++++
he ovary is where oogenesis occurs Ovaries are stimulated by gonadotrophin from the anterior pituitary. Ovaries also have an endocrine function - they release oestrogen and progesterone. The genital tract makes up the rest of the female reproductive system: fallopian tubes take the ova to the uterus. The uterus is a muscular organ, and its mucosal lining undergoes hormone dependent changes. Thevagina is a muscular tube that leads to the outside.
The most internal part of the ovary, the medulla, contains loose connective tissue and blood vessels entering the organ through the hilum from mesenteries suspending the ovary. The medulla has coiled arteries called helicrine arteries.There is no distinct border between the ovarian cortex and medulla.It can be hard to distinguish between the cortex and medulla, but follicles are usually not found in the medulla.

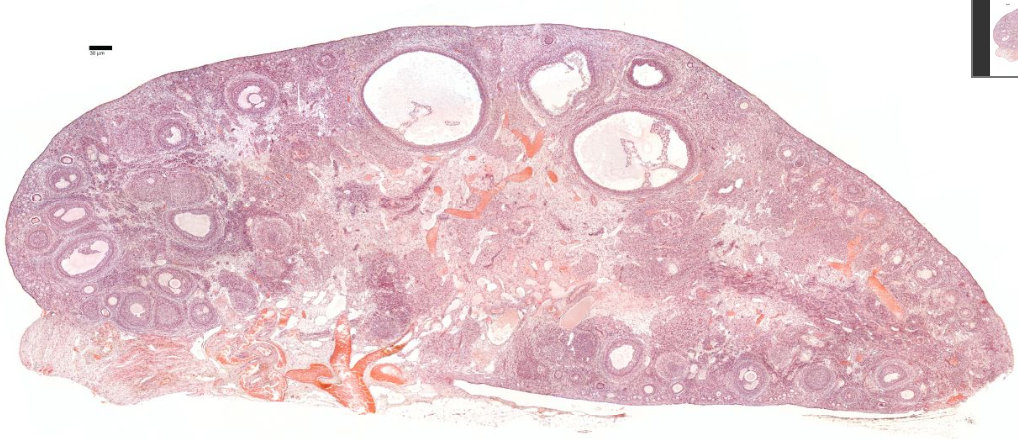
> Next: 02. Oogenesis
A corpus luteum is formed in the ovary during ovulation.During ovulation, an egg is released from a dominant follicle. Following the release of the egg and subsequent fertilization, the follicle seals itself off and forms what is known as a corpus luteum. This mass of cells helps produce the hormone progesterone during early pregnancy.
The corpus luteum will continue to produce progesterone until the fetus is producing adequate levels to sustain the pregnancy, which usually occurs between 7 and 9 weeks of pregnancy.
Progesterone is essential during early pregnancy because:
- it allows the uterus to grow without having contractions
- it supports the growth of the lining of the uterus
- it improves blood flow and oxygen supply
The corpus luteum is supported and maintained by the pregnancy hormone human chorionic gonadotrophin or HCG. The corpus luteum begins to decrease in size at around 10 weeks of pregnancy.
When fertilization or implantation do not occur, the corpus luteum will begin to break down. This causes a decline in estrogen and progesterone levels, leading to the start of another menstrual period.
[The ovaries have a cortex, which is where the ovarian follicles are found, and a highly vascular medulla, with coiled arteries called helicrine arteries.]
The ovaries produce eggs (ova) and hormones such as estrogen and progesterone.
The ovaries are almond-shaped organs of the female reproductive system that produce eggs (ova) and hormones such as estrogen and progesterone. Their structure can be described as follows:
Location
- Positioned in the pelvic cavity, one on each side of the uterus.
- Anchored by ligaments:
- Suspensory ligament: Attaches the ovary to the pelvic wall and contains blood vessels and nerves.
- Ovarian ligament: Connects the ovary to the uterus.
Gross Anatomy
-
Shape and Size:
- Almond-shaped.
- Approximately 3 cm long, 1.5 cm wide, and 1 cm thick, though size can vary.
-
External Appearance:
- Covered by a layer called the germinal epithelium, a thin layer of simple cuboidal cells.
- Below the germinal epithelium lies the tunica albuginea, a dense connective tissue layer.
Internal Structure
The ovary is divided into two regions:
-
Cortex:
- The outer region.
- Contains ovarian follicles in various stages of development:
- Primordial follicles.
- Primary follicles.
- Secondary follicles.
- Mature (Graafian) follicles.
- After ovulation, the remnants of a follicle form the corpus luteum, which secretes hormones.
- Over time, the corpus luteum degenerates into the corpus albicans.
-
Medulla:
- The inner region.
- Contains loose connective tissue, blood vessels, lymphatic vessels, and nerves.
- Provides structural support and nourishment to the cortex.
Blood Supply and Nerve Innervation
- Blood Supply:
- Provided by the ovarian arteries, which branch off the abdominal aorta.
- Venous drainage occurs via the ovarian veins.
- Nerve Supply:
- Sympathetic and parasympathetic fibers contribute to innervation, primarily for regulating blood flow and hormone secretion.
Functional Role
- Gamete Production: Development and release of ova during the menstrual cycle.
- Hormone Secretion: Production of estrogen and progesterone to regulate the menstrual cycle and maintain secondary sexual characteristics.
This highly organized structure enables the ovaries to function as essential reproductive and endocrine organs.
Location
- Positioned in the pelvic cavity, one on each side of the uterus.
- Anchored by ligaments:
- Suspensory ligament: Attaches the ovary to the pelvic wall and contains blood vessels and nerves.
- Ovarian ligament: Connects the ovary to the uterus.
Gross Anatomy
-
Shape and Size:
- Almond-shaped.
- Approximately 3 cm long, 1.5 cm wide, and 1 cm thick, though size can vary.
-
External Appearance:
- Covered by a layer called the germinal epithelium, a thin layer of simple cuboidal cells.
- Below the germinal epithelium lies the tunica albuginea, a dense connective tissue layer.
Internal Structure
The ovary is divided into two regions:
-
Cortex:
- The outer region.
- Contains ovarian follicles in various stages of development:
- Primordial follicles.
- Primary follicles.
- Secondary follicles.
- Mature (Graafian) follicles.
- After ovulation, the remnants of a follicle form the corpus luteum, which secretes hormones.
- Over time, the corpus luteum degenerates into the corpus albicans.
-
Medulla:
- The inner region.
- Contains loose connective tissue, blood vessels, lymphatic vessels, and nerves.
- Provides structural support and nourishment to the cortex.
Blood Supply and Nerve Innervation
- Blood Supply:
- Provided by the ovarian arteries, which branch off the abdominal aorta.
- Venous drainage occurs via the ovarian veins.
- Nerve Supply:
- Sympathetic and parasympathetic fibers contribute to innervation, primarily for regulating blood flow and hormone secretion.
Functional Role
- Gamete Production: Development and release of ova during the menstrual cycle.
- Hormone Secretion: Production of estrogen and progesterone to regulate the menstrual cycle and maintain secondary sexual characteristics.
This highly organized structure enables the ovaries to function as essential reproductive and endocrine organs.

+++++++++++++++
Next is a cortex where the ovarian follicles can be found.
Ovarian follicles are oocytes surrounded by epithelial cells.
Included in the follicles are the cumulus oophorus, membrana granulosa, and the granulosa cells inside it, corona radiata, zona pellucida, and primary oocyte.
The zona pellucida, theca of follicle, antrum and liquor folliculi are also contained in the follicle. Also in the cortex is the corpus luteum derived from the follicles.
{A diagram of a sectioned ovary (a) shows the different stages of follicle maturation, ovulation, and corpus luteum formation and degeneration. All of the stages and structures shown in this diagram actually would appear at different times during the ovarian cycle and do not occur simultaneously. Follicles are arranged here for easy comparisons. The primordial follicles shown are greatly enlarged. The histologic sections identify primordial follicles (b), a primary follicle (c), a secondary follicle (d), and a large vesicular follicle (e). After ovulation, the portion of the follicle left behind forms the corpus luteum (f), which then degenerates into the corpus albicans (g). All H&E.]
+++++++++++++++
he ovary is where oogenesis occurs Ovaries are stimulated by gonadotrophin from the anterior pituitary. Ovaries also have an endocrine function - they release oestrogen and progesterone. The genital tract makes up the rest of the female reproductive system: fallopian tubes take the ova to the uterus. The uterus is a muscular organ, and its mucosal lining undergoes hormone dependent changes. Thevagina is a muscular tube that leads to the outside.
The most internal part of the ovary, the medulla, contains loose connective tissue and blood vessels entering the organ through the hilum from mesenteries suspending the ovary. The medulla has coiled arteries called helicrine arteries.There is no distinct border between the ovarian cortex and medulla.It can be hard to distinguish between the cortex and medulla, but follicles are usually not found in the medulla.


> Next: 02. Oogenesis
During ovulation, an egg is released from a dominant follicle. Following the release of the egg and subsequent fertilization, the follicle seals itself off and forms what is known as a corpus luteum. This mass of cells helps produce the hormone progesterone during early pregnancy.
The corpus luteum will continue to produce progesterone until the fetus is producing adequate levels to sustain the pregnancy, which usually occurs between 7 and 9 weeks of pregnancy.
Progesterone is essential during early pregnancy because:
- it allows the uterus to grow without having contractions
- it supports the growth of the lining of the uterus
- it improves blood flow and oxygen supply
The corpus luteum is supported and maintained by the pregnancy hormone human chorionic gonadotrophin or HCG. The corpus luteum begins to decrease in size at around 10 weeks of pregnancy.
When fertilization or implantation do not occur, the corpus luteum will begin to break down. This causes a decline in estrogen and progesterone levels, leading to the start of another menstrual period.